Fact check: What do we know about the coronavirus delta variant?
The delta variant is now present in more than 80 countries. More transmissible than the alpha variant, it is sparking concerns of further loss of lives and lockdowns.
As India battles a deadly second wave, the UK is seeing COVID-19 cases rise despite vaccinations. Germany is also wary about another wave spurred by the delta variant.
What exactly is the delta variant?
The earliest documented COVID-19 case caused by the delta variant (B.1.617.2) was first found in the Indian state of Maharashtra back in October 2020, and has since then spread widely throughout India and across the world. The World Health Organization (WHO) labelled it a "variant of concern" (VOC) on May 11.
So far, the WHO has identified four VOC: alpha (B.1.1.7), beta (B.1.351), gamma (P.1) and delta.
The delta variant has multiple mutations. Scientists don't know the exact function of these mutations at this point in time but they are associated with allowing the virus to bind to the cells of humans and helping the virus to escape some immune responses, said Deepti Gurdasani, a clinical epidemiologist at Queen Mary University of London.
The delta variant is widespread and has been detected in more than 80 countries so far, according to the WHO. In the UK, tens of thousands of cases have been detected, according to the global science initiative GISAID, which is the highest number of identified delta cases in a country so far.

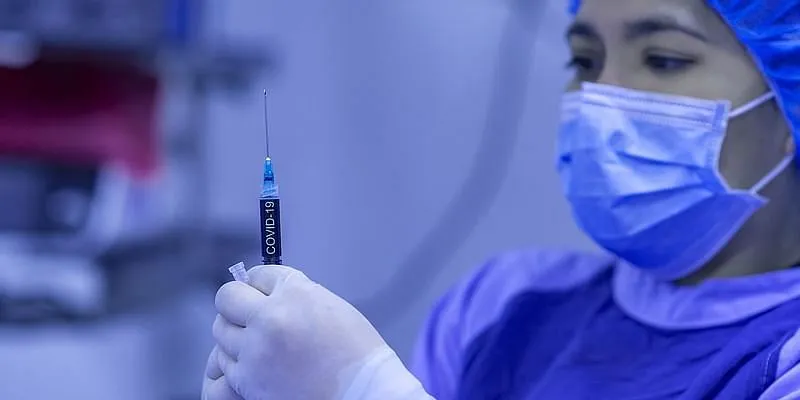
Representational Image
What is the difference between the delta variant and the delta plus variant?
Reports of a more infectious sublineage of the delta variant, sometimes referred to as delta plus or AY.1, have also emerged. This variant has the K417N mutation, which is commonly seen in the beta variant first identified in South Africa. There aren't too many cases of this variant at the moment, according to PANGO Lineages, a website created by scientists that allows users to assign Sars-CoV-2 sequences the most likely lineages.
"This is a mutation that has possibly been associated again with better escape from vaccines and possibly even increased transmissibility," said Gurdasani. "We don't yet know the properties of this new variant with this particular mutation on top."
Is the variant more infectious?
Data from Public Health England (PHE), an executive agency of the UK's department of health, indicates that more than 90% of new COVID-19 cases in the UK are from the delta variant.
The UK had confirmed more than 42,000 cases of the delta variant as of June 9, with an increase of nearly 30,000 reported from June 2-9. Of the cases confirmed by PHE, most were either not vaccinated or had only had one vaccine dose.
PHE research found that the delta variant is associated with a 64% increased chance of household transmission compared to the alpha variant (B.1.1.7) first identified in the UK.
"What we noticed early on in India was that [the delta] variant was outcompeting or growing faster than the so-called Kent or alpha variant that first originated in the UK," said Gurdasani, "and this was very concerning because we knew at that point in time that the alpha variant was already more transmissible than the original virus."
Is it deadlier?
There is still little data available about whether the delta variant causes more deaths.
There were 42 deaths caused by the delta variant in the UK between February 1 and June 7. Of these, 23 people were not vaccinated, seven died more than 21 days after their first vaccine dose, and 12 died more than two weeks after their second dose.
Compared to the alpha variant, the delta variant is more likely to cause hospitalization, according to PHE.
More than 1,300 people were admitted to hospital for all COVID-19 variants from June 7-13, an increase of 43% from the previous week.
Both the Pfizer-BioNTech and AstraZeneca vaccines are slightly less effective at preventing hospitalization in people with the delta variant compared to those with the alpha variant.
The Pfizer-BioNTech vaccine is 6% less effective for the delta variant after two doses and AstraZeneca is 1% less effective, according to a PHE preprint.
"The data from the UK tells us that it is more likely to cause hospitalization, so it wouldn't be surprising if it is found to be more deadly," said Gurdasani.
While further work needs to be done to determine the level of protection against death from the delta variant, PHE said it is expected to be high.
"While vaccinations in countries where these are widely available may avert some of this, that connection between case and hospitalizations is still not going to be lost," Gurdasani said, "and we know that the majority of the world still has a large, unprotected population that hasn't been vaccinated yet."
More information is needed to confirm studies and reports that say the delta variant causes more severe disease, said the WHO's COVID technical lead Maria Van Kerkhove.
"We need more information to determine: is it really the variant itself or is it a combination of factors?" Van Kerkhove said.
Do the vaccines protect us from the delta variant?
A PHE study awaiting peer review found that the Pfizer-BioNTech vaccine was 94% effective against hospitalization after one dose and 96% effective against hospitalization after two doses. AstraZeneca was 71% effective after one dose and 92% effective after two.
Efficacy against symptomatic disease from the delta variant for Pfizer-BioNTech was 36% after one dose and 88% after two doses. For AstraZeneca it was 30% after one dose and 67% after two.
"This doesn't mean that there is no protection," says Gurdasani. "But there is definitely a reduced protection against just infection or asymptomatic mild disease, particularly with one dose, but also with two doses."
Is the delta variant responsible for the pandemic situations in India and the UK?
Whether the delta variant is mainly responsible for the situation in India cannot be scientifically proven yet. More testing and sequencing would be needed for this.
But India is one of the countries worst affected by the pandemic. More than 29 million cases have been registered so far, according to Johns Hopkins University, and the health system is hugely overburdened.
Clinical epidemiologist Gurdasani says that in addition to the spread of the mutation, several factors have played a role in the massive spread of the coronavirus in India.

Image Source: Unsplash
"I think it's been a combination of very late action by governments to put basic public health measures in place and overconfidence that herd immunity had been reached prior to this," said Gurdasani.
In the UK, the situation has deteriorated drastically. The 7-day incidence rate for all COVID-19 infections was below 20 at the beginning of May, but has since risen to more than 70 new infections per 100,000 people within a week.
A total of 55,216 cases from June 10-16 represent an increase of almost a third compared to the previous week.
How can we protect ourselves from the variant?
Rules like keeping a distance of 1.5 meters, washing hands, wearing masks and ventilation protect against all known variants of the coronavirus including delta, Germany's Robert Koch Institute (RKI) told DW.
Travelling to so-called virus-variant areas should be avoided as it has increased the spread of the coronavirus and its variants since the beginning of the pandemic. That is why comprehensive quarantine rules are needed, Gurdasani said.
The WHO's Van Kerkhove said on Twitter that public health and social measures "need to be used strategically and must be supported by governments, communities and individuals to stop all variants of the virus."
What are the symptoms of the delta variant?
According to data from the UK's ZOE COVID Symptom Study app, the symptoms caused by the delta variant differ from the ancestral virus and other mutations. As people in the UK with COVID-19 reported their symptoms to the ZOE app, they described headaches, sore throats, runny noses and fever. In some cases, there was coughing as well.
"It's more like a bad cold for the younger population," says scientist and co-founder of the app Tim Spector.
This could lead people to think they only have a mild cold and continue to go about their day normally. People with these symptoms should stay home and get tested, says Spector.
(This article by Louisa Wright and Kathrin Wesolowski was originally published on Deutsche Welle.)
Edited by Anju Narayanan









![[Exclusive] Vauld to seek 3-month moratorium extension as creditors panel explores bailout options](https://images.yourstory.com/cs/2/a09f22505c6411ea9c48a10bad99c62f/VauldStoryCover-01-1667408888809.jpg)
