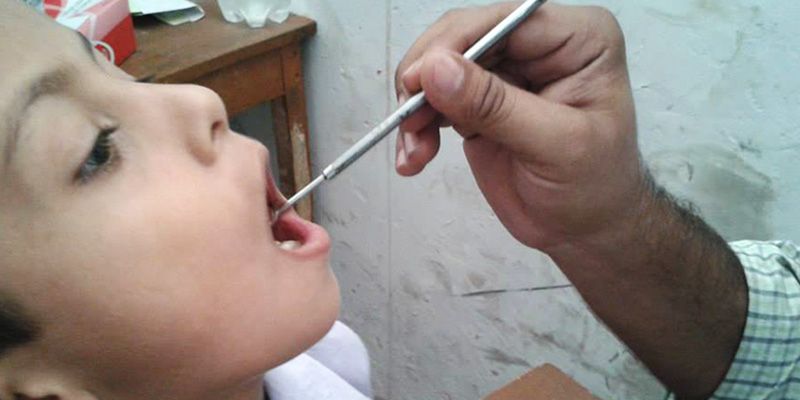
Shelley Saxena’s journey from managing a multi-million dollar product portfolio at IBM to founding Sevamob
Shelley Saxena was a product manager at IBM, managing a multi-million dollar product portfolio when he decided to quit and co-found Saasmob, a mobile technology company in 2009. Saasmob provided advisory services through mobile applications to farmers in the United States, via the University of Tennessee and University of Georgia. Shelley, who is originally from Lucknow, had studied engineering at IIT Roorkee, and went on to get an MBA from Cornell University.
Shelley wanted to replicate the Saasmob model in India, but due to high illiteracy rates and low penetration of data-capable smartphones in their target audience, they had to deploy field teams. This meant an increase in costs that was unrelated to the original model. In order to cover the cost of these teams, they did some market research on services that users would be willing to pay a monthly subscription for. Healthcare emerged as a service that 80 per cent were willing to pay for. The epiphany lead them to start a healthcare and advisory service, and slowly after gauging the potential, they started to double-down on the healthcare space, concentrating majority of their efforts there.
The result? The launch of Sevamob in 2011 to leverage technology to deliver healthcare services more efficiently to customers from the bottom of the pyramid.
The problem and the solution:
India lags behind on most indicators linked to health. The average life expectancy is 66 years, and ranks at a lowly 127th position out of 180 countries. On indicators like infant mortality, child malnutrition and maternal mortality, it fares worse than some Sub-Saharan African countries. It has one hospital bed for 879 individuals versus World Health Organisation recommendation of 1.9 beds per 1,000 population.
The Indian government spends just 4 per cent of the GDP on healthcare, leading to most of the expenditure or 61 per cent coming out of the individual’s pocket. There is even greater disparity in low-income communities, where there is limited access to primary healthcare. In rural areas and smaller cities, the main source of primary care is government-run primary healthcare centers. In many areas, these are understaffed and over-crowded and often have touts who act as commissioned agents of city-based service providers.
Sevamob provides primary healthcare services in tier two, three and four cities via mobile clinics as well as a tele-health marketplace. Their target audience includes students, employees or groups whose monthly family income is between Rs 5,000 to Rs 25,000. In some areas that SevaMob serves, there are no registered doctors in a 10 km radius.
But just having a service that is affordable is not enough. Sevamob’s target audience have limited awareness about the need for regular primary care. Even though early interventions can help avoid, contain and even cure diseases, people often visit a doctor when something drastic happens. Shelley believes that this is a key reason why average life expectancy in India is 66 years versus 78-80 years in developed economies. He hopes that Sevamob can play a small role in increasing awareness and improve healthcare indicators in the long term.

Sevamob subscription-based payment model:
Sevamob’s mobile clinics provide basic primary care, medicines for common ailments and prescriptions on groups’ premises. More advanced care is provided by a 24×7 call center and back-office appointments.
For catastrophic care, Sevamob bundles cashless hospitalization benefits and accident insurance. The basic subscription plan, which includes home-based primary care and accident insurance costs Rs. 100 a month. For an additional Rs. 50 every month, the premium plan includes insurance of up to Rs. 30,000 to cover in-patient care.
In January this year, they started a tele-health marketplace that enables patients to get video consultations, second opinions and in-clinic appointments from participating healthcare providers. This reduces the need for a patient to travel to a large hospital to get a diagnosis.
Sevamob’s low-cost healthcare delivery model works on a hub-and-spoke model with appropriate skill-set matched at each touch-point.
Sevamob’s success and challenges:
At present, they service in excess of 5,000 subscribers in Uttar Pradesh, Karnataka and the National Capital Region. They have also expanded overseas and replicated the model in Liberia.
“Each satisfied customer testimonial, every new launch, every award, each funding round brings us lots of smiles. On the other hand, making sure that we serve our customers with a high quality of service and at the same time deploy investors’ money wisely keeps us up at night,” says Shelley.
But like most startups that are trying to grow, they have their fair set of hiccups. Major challenges include obtaining capital for expansion and maintaining a high quality of service as they grow rapidly. “For the former, we are blessed with very entrepreneur friendly social impact investors. For the latter, we use specific rotations and protocols, technology and the call center to maintain and track quality of care,” explains Shelley.
Sevamob also did a small pivot. After initially serving only rural customers, Sevamob tweaked its model and spread to urban areas after they were not able to achieve a sustainable patients per doctor per day ratio. Switching to a group model of subscription in Tier 2,3 and 4 cities, but keeping the target income-segment (Rs. 5,000 to Rs. 25,000 monthly) the same, has worked better for Sevamob.
Future big goal:
“Within five years, our target is for more than 1 million mobile clinic subscribers and 37.5 million marketplace users. We also want to replicate the model in additional geographies via licensees,” predicts Shelley.